I was recently asked to write a short blog on where I think the most progress has been made in my field of research. It was part of Dementia Researcher’s contributions to World Alzheimer’s day and it got me thinking. I found myself pondering beyond the topic of progress in my field. Instead, I found myself thinking about dementia research as a whole and how our approach to dementia has changed with our constantly increasing knowledge. This is the topic I want to blog about this month; the diversification of our thinking around dementia.
There was a time when dementia was not understood at all. Until the late 19th century, a person exhibiting signs of dementia was unlikely to get medical treatment. Instead, they would be condemned to the brutal asylums that existed for many centuries, into the 1960s and 1970s. It is a prime example of what can happen when incorrect scientific assumptions are not challenged and widely circulated and accepted. Fortunately, a new wave of thinking began to challenge then norm in 1906 when Alois Alzheimer presented his findings on a condition that would later be called Alzheimer’s. At the time, his discovery was not fully appreciated and his presentation at a scientific conference was virtually disregarded with the audience rushing him off to hear the next lecture.
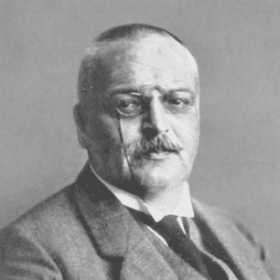
Alois Alzheimer was a German psychiatrist and neuropathologist and a colleague of Emil Kraepelin. Alzheimer is credited with identifying the first published case of “presenile dementia”, which Kraepelin would later identify as Alzheimer’s disease.
Fast-forward a century and we now know exponentially more about diseases like Alzheimer’s. Patients are no longer banished to Bedlam. There is no more “grandad just went mad in his old age”. Thanks to outreach initiatives like Alzheimer’s Research UK’s ‘Share the Orange’ the majority of people now understand that dementia is not a normal part of aging. It is a disease that we can strive to diagnose, prevent and fight. But our knowledge has progressed in another way as well.
When Alois Alzheimer first observed fundamental changes in the post-mortem brains of Alzheimer’s patients, the data he presented suggested diseases like Alzheimer’s were purely diseases of the brain.
For decades the problem of dementia was approached with a mind-set of “this is a disease that manifests in the brain… let’s focus on the brain”. We forgot that our body is a connected network of organs that work together. Nothing works in segregation. A lot was learned by looking solely at the brain but I am glad to see that as we moved forward, we started looking outside of the brain for answers as well. Unsurprisingly, we found a large number of mechanisms outside of the brain that can contribute to dementia and I would like to share a select few now as a testament to how far our knowledge has come from the days of locking people in asylums.
Perhaps one of the most commonly known examples is the link between dementia and diabetes. In type 1 diabetes, patients simply cannot produce the insulin required to regulate their blood sugar but in type 2, the insulin is there but it is unable to do its job properly. We covered this in a recent podcast about another exciting field; diet and dementia but I’ll let you listen to that yourself rather than read it here. Back to the topic at hand; the insulin resistance. We now know this has implications on the brain. Insulin is also involved in the formation of the junctions between brain cells that we call synapses. Cells within the memory region of the brain interact with insulin, giving it a major role in memory formation. Insulin, therefore, seems to have a part to play in normal brain function. Insulin resistance in brain cells can lower the ability of the hormone to maintain healthy brain cells, leading to memory loss and dementia.
So it seems the pancreas can have a role to play in developing dementia and it doesn’t stop there. The kidneys may also be implicated. Earlier this year a 5-yearlong study correlated decreased kidney function with increased dementia risk. The mechanisms are still being unpicked but the evidence presented seems pretty compelling. And if we look further south, the colon is also seemingly involved in dementia. More specifically, the billions of bacteria that reside in our gut; the gut microbiome (which is significantly altered in dementia patients). This is actually a topic for an upcoming podcast so keep your eyes peeled for that!
These are just a few examples too. The heart, liver, lungs… basically pick and organ and you can probably find studies showing their potential roles in dementia pathogenesis. It may make the issue seem insurmountable but to me, it represents the amount of progress we have made in unpicking this hugely complex issue. If we continued to just look at the brain we would know far less than we do now and be further from any real breakthrough. It’s like rearranging the furniture in your home. You get to a point where everything is all over the place and you feel overwhelmed but shortly after, things start to fit into place and it all makes sense. As we push forward, the image may get a bit more chaotic but it will all fit into place eventually.
Did you know that we also publish all of our blogs into their own podcast feed? So you can listen even when you’re on the move – find them here, and hit subscribe Podbean, Spotify, Apple Podcasts

Dr Sam Moxon
Author
Dr Sam Moxon is a biomaterials scientist at the University of Manchester. His expertise falls on the interface between biology and engineering. His PhD focussed on regenerative medicine and he now works on trying to develop 3D bioprinting techniques with human stem cells, so that we better understand and treat degenerative diseases. Outside of the lab he hikes through the Lake District and is an expert on all things Disney.

 Print This Post
Print This Post




