When you hear the word “dementia” it is common to think about the symptoms from a few different angles. You might think of the mental side of dementia. Loss of memory, confusion and hallucinations to name a few. It is possible that you also consider the physical aspects of the disease like appetite and weight loss. Perhaps you will also think of the biology that underlies the progression of dementia. The build-up of toxic proteins and subsequent loss of brain cells and matter. One thing you are unlikely to think of is a mechanical side to dementia. It is not really widely publicised but it is definitely something that is observed in dementia patients.
So what do I mean by the “mechanical” effects of dementia. I am referring to the mechanical properties of the brain; specifically how “stiff” it is. Every tissue in our body has a defined stiffness. Bone, for example, is classified as having a high stiffness because it is very strong, firm and can withstand very high impact. It has to in order to be able to carry out its main functions of keeping us upright and protecting our much softer vital organs from impact damage. In contrast, the brain is an extremely soft and fragile tissue. That is why our skulls are so thick. We need to protect our brains from damage.
Tissue stiffness is very closely controlled in our bodies and the cells embedded within our tissues are as much in control of tissue stiffness as they are controlled by it. Stiffness is one of the many properties in our body that is regulated by an intricate and elegant balance of homeostasis. Any healthy patient should be exhibiting tissue stiffness’ within the normal range. Certain disease have, however, been shown to correlate with a change in tissue stiffness. Many cancers, for example, result in an increased tissue stiffness as the tumour cells grow and remodel their environment to become more “tumour friendly”. In breast cancers, it is common to see fibres of collagen become denser and more aligned than normal, resulting in increased breast tissue stiffness.
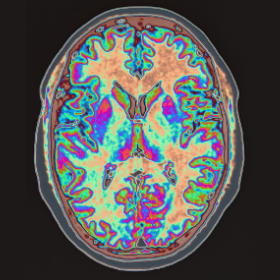
Magnetic Resonance Elastography – is not the stuff of sci-fi
Interestingly, medical evidence is now also pointing towards dementia as being another healthcare issue that results in changes in tissue stiffness. However, the picture is a little more complex than the stiffness always going either up or down. It appears it depends on what dementia-causing disease is present in the patient. In Alzheimer’s for example, the brain is often seen to become significantly softer than normal. That is not surprising given that Alzheimer’s results in the death and loss of brain cells and tissue. You would expect the brain to become mechanically weaker as a result. Conversely, in dementias with an integral vascular complication, many studies have shown that the blood vessels within the brain actually become stiffer as they become more hypertensive. Either way, these changes in stiffness could provide ways of diagnosing dementias earlier than we can now. Normally a patient is not diagnosed until the neurodegenerative mechanisms playing out in their brains become advanced enough to manifest as physical or mental symptoms. At this point a considerable portion of the brain has already been lost. Being able to screen for more subtle changes in brain tissue stiffness could alert medical professionals to early signs of dementia progression, allowing therapies to be administered before large scale damage is done. This would have a major impact on the lives of dementia patients.
So I guess the big question is how do we go about screening for it? Normally in a lab if you want to probe the stiffness of a material you have a range of equipment to use from rheometers and compression testers to atomic force microscopes. However, you can’t really cut someone’s head open and take a sample of brain tissue to measure the stiffness and determine brain health. It’s a bit counterintuitive! It turns out the answer lies in something that is used in hospitals every day. Magnetic resonance imaging (MRI) is commonly used to examine tissue health and is a key diagnosis tool for dementia. If MRI is combined with low frequency vibrations it allows practitioners to get an “elastic map” of a tissue. The process is called magnetic resonance elastography (MRE) and it can detect regional changes in brain stiffness without having to cut a patient open.
It’s a powerful tool and could have a big role to play in improving the speed and accuracy with which we diagnose and treat cognitive impairment. I am definitely not saying drop everything else and just focus on this but, with so many questions still remaining about how we can better understand and treat dementia, why not use all the tools we have? Tissue stiffness changes are one of many manifestations of dementia. It is good to see it being given the consideration it warrants in the ongoing discussion about how we can fight to eradicate neurodegeneration for good.
Author

Dr Sam Moxon
Dr Sam Moxon is a biomaterials scientist, and his expertise falls on the interface between biology and engineering. His PhD focussed on regenerative medicine and he now works on trying to improve on culture techniques for human stem cells, so that we can gain a better understanding of how diseases like Alzheimer’s manifest. His work at The University of Manchester looks at 3D bioprinting with stem cells. Outside of the labhe hikes through the Lake District and is an exert on all things Disney.
Have you used magnetic resonance elastography ? Reply in the box below

 Print This Post
Print This Post




