Dementia is rarely considered a market issue, well at least not explicitly. Yet the unequitable distribution of care and support, cost of care and unpaid care, and inequality of information are symptoms of a ‘failed market’. This is according to the Treasury’s Green Book which identifies four domains of market failure: under-provision of public goods/services, imperfect information about goods/services, externalities, and market or monopoly power.
Market failure is when market forces cause poorer societal welfare (Finch et al., 2020). For example, the universal availability, marketing, and pricing of unhealthy foods which has driven an obesity epidemic. However in dementia, the opposite phenomenon exists. Rather than the universal distribution of goods that cause harm, we have the under and unfair provision of goods and services that alleviate and prevent harm.
There is much to learn from the market in which dementia functions, albeit dysfunctional. Taking a market failure approach through regulation, taxation, and distribution could improve population health and reduce inequalities. In this longer than usual read I argue why a ‘nanny state’ (overprotective government) is necessary and consider two key levers for change, revenue and regulation.
Revenue and redistribution
Health and Social Care are a common good like policing and schooling and are funded in the UK through public revenue, mainly taxes. If public budgets and tax levels change so do revenues. Not increasing taxes while simultaneously cutting health spend is therefore an effective formula for crashing health systems. A double jeopardy recurrently reinforced through the politics of our economy.
In recent decades the UK has ignorantly prided itself on small state politics, low taxes, and in recent years, fiscal conservatism, dramatically cutting 40% funding to Local Authorities who provide crucial Adult Social Care services. This has meant people eligible to draw on Social Care, such as those living with dementia, have found it increasingly difficult to get publicly funded care despite rhetoric of personalisation.
Additionally, the fact that, unlike other non-communicable diseases such as cancer and heart disease, dementia is considered a Social Care issue (i.e. means tested) enforces an unwritten ‘dementia tax’. Two thirds of the £34.7 billion a year cost of dementia is borne by people self-funding their care (families pay over 60% of costs) and unpaid carers such as family and friends providing unpaid labour with an annual value of £13.9 billion. People have to draw on family and friends or surrender the vast majority of their savings and even their assets to sustain their care at home.
The Health and Social Care Levy was a promising tax reform raising billions to reform how people pay for care to try and address these market issues. However this potentially long-term tax-based solution has since been binned, and it remains unclear how reforms will now be funded. This is despite growing public support for increased taxes to fund better public services, with a Net Wealth Tax on the richest in society being the number one choice for raising revenue (41% in favour). This shows a clear appetite for policies that redistribute the wealth in our society more equitably, to redress the wealth gap between the richest 10% and everyone else, which has continued to widen despite the pandemic.
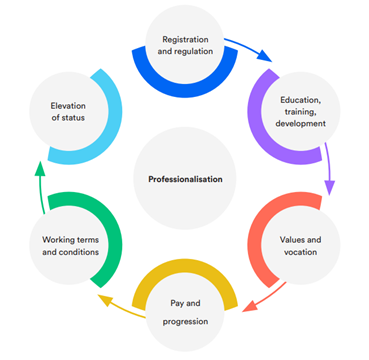
The concept of professionalisation of care workers has been proposed as a solution to these market issues
Regulation
Health systems have not escaped the negative effects of free market fundamentalism. The aggressive outsourcing of contracts to deliver dementia wellbeing services, cafes, and other state-funded services, for examples, has been damaging. For example, a focus on reducing costs negatively impacts quality, and introducing a culture of competition has led to de-regulation and casualisation of the Adult Social Care workforce with stagnant wages and dangerous working conditions.
The concept of professionalisation of care workers has been proposed as a solution to these market issues. A report published earlier this year highlights the lessons England can learn from other countries who have implemented measures to drive professionalism, including Scotland and Wales. The report is unequivocal. Implementing a range of measure including professional regulation for care workers, high-quality training in specialist areas like dementia, improved pay, working conditions, terms and conditions will lead to better quality care, lower rates of staff turnover, and address entrenched labour inequities affecting woman and BAME communities who make up a significant amount of the workforce.
In real terms, professionalisation could result in care workers having more comprehensive and managerial roles as case managers like in Japan where standards are high. Or parity of pay with other professionalised workforces like Australia who are paid at least $19 per hour.
An uncharacteristically optimistic end
Market failure occurs when the distribution of goods and services in the market is ineffective. In dementia, and health more generally, the symptoms of market failure are all around us, from workforce issues and equity of access, to falling living standards and reversing life expectancy. Unfortunately, we have become all too familiar and in some cases content with health markets being imperfect.
The politically motivated individualistic framing of health and, ironically, the national debt, have wrongly dominated public discourse and opinion thus far, making it incredible difficult to whip-up support for macro-level intervention such as increased taxation and regulation. A big reason being these measures are seen as trespassing on people’s autonomy and freedoms. Why should I pay more taxes for people who chose to be homeless, sick, or unemployed? But society is beginning to account the costs and question the sustainability of capitalism.
If you’re finding it hard to imagine how the market could start to work for people and not just the ruling class, look to the sugar tax and smoking ban for optimism. These healthy public policies, while initially thought of as radical and politically unpopular, have proved to be highly effective at improving population health with a cost-saving element for the state. In this world, National (Public Health) Service may even be politically palatable.
Nathan

Nathan Stephens
Author
Nathan Stephens is a PhD Student and unpaid carer, working on his PhD at University of Worcester, studying the Worcestershire Meeting Centres Community Support Programme. Inspired by caring for both grandparents and personal experience of dementia, Nathan has gone from a BSc in Sports & Physical Education, an MSc in Public Health, and now working on his PhD.

 Print This Post
Print This Post




